Table of Contents[Hide][Show]
Intercostal neuralgia can cause chronic ribcage pain that limits daily activities and may prevent employment, making long-term disability (LTD) benefits critical. This guide explains the condition, its symptoms, and treatment options, and outlines how long-term disability insurance works. It details eligibility requirements, the medical documentation needed, and the step-by-step application process, with strategies to overcome common challenges. It also includes legal assistance for appeals and guides patients to more resources for continued help.
Understanding Intercostal Neuralgia
Intercostal neuralgia is a chronic nerve pain condition that affects the intercostal nerves, which run along the ribcage between the ribs. When these nerves become irritated, inflamed, or damaged, the resulting pain can be severe and persistent.
Common Symptoms
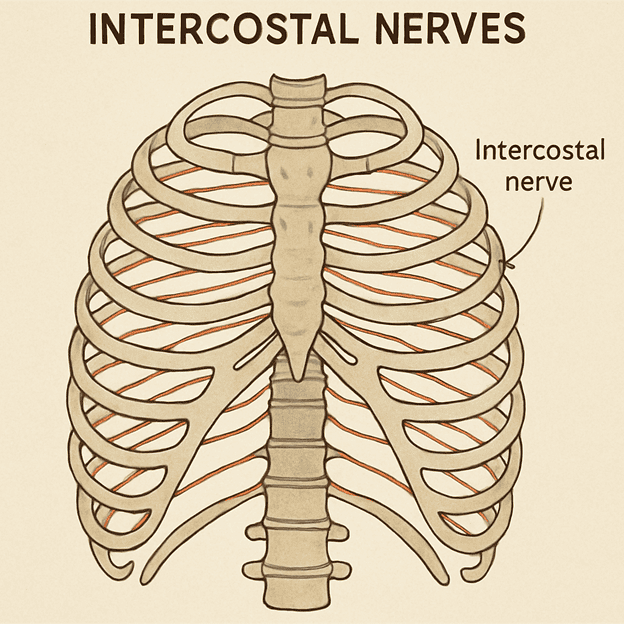
People with intercostal neuralgia may experience one or more of the following symptoms:
- Sharp, burning, stabbing, or aching pain along the ribcage
- Pain that follows the path of one or more ribs
- Constant pain or pain that occurs in episodes
- Increased pain with movement, including twisting, reaching, or lifting
- Worsening pain with deep breathing, coughing, or sneezing
- Tenderness or heightened sensitivity along the chest wall
- Pain that interferes with posture, sitting, or prolonged standing
Because the intercostal nerves play a role in breathing and upper-body movement, these symptoms can significantly interfere with daily activities. Even routine tasks such as bending, sitting for extended periods, or maintaining a consistent work position may worsen pain and make sustained work difficult.
Understanding intercostal neuralgia is important for proper diagnosis and treatment planning. Clear documentation of symptoms, triggers, and functional limitations can also be critical when discussing the long-term impact of the condition with healthcare providers.
Neuralgia Treatment Options
Treating intercostal neuralgia involves addressing pain and improving function. Various strategies exist, each offering unique benefits. A combination of treatments often yields the best results.
- Medication is a common first step. Pain relievers, anticonvulsants, or antidepressants might be prescribed to manage symptoms. Each medication targets specific elements of the pain pathway.
- Physical therapy plays a crucial role in treatment. Exercises can enhance mobility and reduce pain. Therapists design personalized programs focusing on strengthening and flexibility.
- Advanced interventions include nerve blocks. These involve injecting anesthetic near the affected nerves, offering temporary pain relief.
Beyond traditional options, lifestyle changes support pain management. Individuals may find relief through:
- Mindfulness and relaxation techniques.
- Ergonomic adjustments at home or work.
- Regular gentle exercise, such as swimming or walking.
- Maintaining a healthy diet to support nerve health.
Effective treatment requires a holistic approach, addressing both physical and emotional symptoms. Psychological support, such as counseling, can be beneficial. This helps patients cope with the ongoing challenges of chronic pain.
Consulting a multidisciplinary team ensures comprehensive care. Pain management specialists, therapists, and counselors can collaborate to tailor the most effective plan. Regular follow-ups allow adjustments to treatments as needed, supporting ongoing symptom management.
Long-Term Disability for Intercostal Neuralgia
Intercostal neuralgia often does not improve and may worsen over time. The condition can lead to ongoing nerve pain in the ribs and chest. This can make it hard to work regularly and dependably. Jobs that need you to sit, stand, twist, reach, or stay focused for a long time can be hard when pain comes on suddenly or makes it hard to move.
In addition to chronic pain, intercostal neuralgia can interfere with concentration, focus, and stamina. Ongoing pain often disrupts sleep and leads to fatigue, reduced mental clarity, and difficulty staying on task. Over time, these limitations can also contribute to emotional strain, including anxiety or depression.
If you have intercostal neuralgia and cannot work regularly, you might qualify for long-term disability benefits.
What Is Long-Term Disability Insurance?
Long-term disability insurance provides financial assistance when a medical condition prevents work. It’s designed to replace a portion of your income when illness or injury impairs your earning ability.
Typically, these policies cover a wide range of conditions. This includes those causing long-term or permanent disability. Intercostal neuralgia, with its debilitating pain, often qualifies if it stops gainful employment.
The insurance works by paying a percentage of your salary. Payouts can range from 50% to 70% of your income, depending on the policy. Benefits usually start after a waiting period, termed the “elimination period.”
Understanding the specific terms of a policy is crucial. Look out for:
- The definition of disability under your plan.
- Elimination period length before benefits start.
- Duration of benefits payments.
- Any exclusions, such as pre-existing conditions.
Having this coverage ensures you won’t deplete savings when health prevents working. It offers peace of mind, allowing focus on health recovery rather than financial strain. Policies vary, so consulting with an insurance professional is often beneficial. This ensures coverage aligns with personal needs and circumstances.
Eligibility Criteria for Long-Term Disability Benefits
Eligibility for long-term disability benefits hinges on meeting certain criteria. These criteria differ among insurance providers and policies. To qualify, comprehensive medical documentation and evidence of impairment are crucial.
A main requirement is showing how serious the condition is. Insurers need to see that intercostal neuralgia significantly impacts daily life. This includes hindering routine activities and preventing work tasks.
Documentation often involves detailed medical reports. These should outline diagnosis, symptoms, and treatment history. Regular follow-ups with healthcare professionals are essential to keep records updated.
Common eligibility criteria include:
- Documentation of impairment and diagnosis.
- Treatment history and outcomes.
- Evidence of work impact or inability to perform job duties.
- Proof the condition is expected to last a specific duration.
Insurance companies may also look at a person’s ability to do different kinds of work. This is usually assessed through functional and vocational evaluations. These evaluations help find out how earnings might be affected.
Navigating these criteria can be challenging. You may need to work with healthcare providers and legal experts. Understanding policy details ensures no important criteria are overlooked, improving approval chances.
The Application Process for Disability Benefits
Applying for disability benefits involves several detailed steps. First, look over your long-term disability policy. Understanding the specific terms and conditions is essential.
Next, gather all relevant medical documentation. This includes notes from doctors, test results, and any treatment plans. Comprehensive medical records support your claim’s credibility.
The application form is crucial and must be completed accurately. Missteps or omissions can lead to delays or denials. Include all necessary personal, employment, and medical details.
After submission, patience is key. The review process can be lengthy. Keep communication lines open with your insurer, responding promptly to any requests for more information.
Key steps in the application process:
- Review insurance policy details.
- Collect comprehensive medical records.
- Complete application forms accurately.
- Maintain open communication with insurers.
A streamlined approach to the application process improves the chances of success. Following each step carefully ensures your claim is comprehensive and reduces the risk of errors.
Medical Documentation and Evidence Requirements
Medical documentation serves as the backbone of a successful disability claim. Insurers need clear evidence demonstrating the severity and impact of intercostal neuralgia. Without this, your claim may be at risk.
Ensure your documentation captures detailed medical history. Include diagnosis reports, treatment plans, and summaries of medical visits. Each document should illustrate how neuralgia hinders your daily life and ability to work.
Consistency in medical documentation strengthens your claim. Regular follow-ups with healthcare providers can demonstrate the persistence of your condition. Detailed notes on treatments and responses bolster your evidence.
Non-medical evidence can also support your claim. Personal statements or affidavits from family or employers can provide additional insight. They often reflect the real-world impact of your condition.
Key elements of strong documentation:
- Comprehensive medical reports.
- Regular updates from healthcare providers.
- Clear evidence of functional impact.
- Supporting statements from personal contacts.
Thorough documentation paves the way for understanding your reality. It highlights your condition’s influence on everyday tasks and your ability to work, guiding the insurer’s evaluation.
Common Challenges and How to Overcome Them
Pursuing disability benefits for intercostal neuralgia can be daunting. Applicants often face several hurdles throughout the process. Knowing these challenges and strategies to tackle them can be crucial.
One common issue is insufficient medical evidence. Claims can be denied if documentation does not clearly show the severity of your condition. Ensure thorough and consistent medical records to address this problem.
Miscommunication with insurance providers is another hurdle. Complex terms and procedures may seem overwhelming. Keeping clear records of all communications and seeking clarification when needed can be helpful.
Navigating policy details can also be challenging. Insurance plans often contain specific clauses and conditions. Knowing your policy well helps you avoid surprises and makes it easier to prepare a strong claim.
Tips to overcome these challenges:
- Maintain thorough medical records.
- Clarify any confusing correspondence.
- Understand every detail of your insurance policy.
- Seek professional advice if needed.
Proactively addressing these issues can streamline the disability claim process. Preparation and knowledge are key components in overcoming these obstacles and ensuring a smooth experience.
Legal Support and Appeals for Denied Claims
Facing a denial of your disability claim can be discouraging. However, legal support can enhance the chances of a successful appeal. Understanding when and how to seek help is vital.
Hiring an attorney with expertise in long-term disability claims can make a difference. They provide insight into complex legalities and negotiate effectively on your behalf. This professional assistance can simplify the appeals process.
The appeals process involves several key steps. It is important to meet all deadlines and send in the necessary documents on time. Legal experts can make these processes easier and make sure nothing is missed.
Steps in handling denied claims:
- Understand the denial reasons.
- Collect additional supporting medical evidence.
- Submit a comprehensive appeal letter.
- Work closely with your attorney throughout the process.
Getting a lawyer helps you feel more secure and organized with your appeal. It can significantly improve your prospects of obtaining the benefits you need.
Additional Resources and Support for Patients
Coping with intercostal neuralgia can be challenging. However, patients are not alone in this journey. Various resources and support networks are available to help manage the condition and navigate life changes.
Joining peer support groups can provide emotional relief and valuable insights. These communities foster connections with others facing similar challenges. They can offer advice and share experiences related to treatments and coping strategies.
Online platforms and forums are also beneficial. They connect people globally, offering support and information. Additionally, resources from medical organizations can guide treatment and provide up-to-date research on intercostal neuralgia.
Possible resources for patients include:
- Local support groups and meet-ups
- Online communities and forums
- Healthcare provider recommendations
- Educational resources from medical institutions
By leveraging these resources, patients can enhance their quality of life and find solace in community support. Keeping informed and connected is crucial for overall well-being and effective management of intercostal neuralgia.
Call Ortiz Law Firm Today for a Free Case Evaluation
Living with intercostal neuralgia can make working consistently difficult, and navigating the long-term disability process on your own can feel overwhelming. Understanding your rights and options is an important first step toward protecting your income.
Our experienced disability attorneys know how challenging long-term disability claims can be, especially when you are dealing with ongoing pain and an uncooperative insurance company. Ortiz Law Firm may be able to help you pursue long-term disability benefits for your condition.
Call us today at (888) 321-8131 for a free case evaluation with a member of our team.
Sources
- Healthline. “Intercostal Neuralgia” Retrieved from: (http://healthline.com/health/intercostal-neuralgia) Accessed on February 9, 2026
- WebMD. “What to Know About Intercostal Neuralgia” Retrieved from: (https://www.webmd.com/pain-management/what-to-know-intercostal-neuralgia) Accessed on February 9, 2026

